What is FHIR and how is it used in data mapping?
- Home
- Insights
- Article
- What is FHIR and how is it used in data mapping?
Qualitative Research Service
- What is FHIR (Fast Healthcare Interoperability Resources)?
- Why FHIR Matters in Healthcare Data Interoperability
- What is Data Mapping in Healthcare?
- How FHIR is Used in Data Mapping
- Benefits of FHIR Data Mapping
- Real-World Applications of FHIR Data Mapping
- Challenges in FHIR Data Mapping
- Best Practices for Effective FHIR Data Mapping
- Conclusion
News & Trends
Recommended Reads

Data Collection
As the data collection methods have extreme influence over the validity of the research outcomes, it is considered as the crucial aspect of the studies
- 1. Introduction
- 2. DeepHealth’s Diagnostic Suite™: Revolutionizing Radiology Workflows
- 3. Key Features
- 4. AI Impact on National Screening Programs
- 5. SmartMammo™: Enhancing Breast Cancer Screening
- 6. DeepHealth AI Use Cases Across Specialties
- 7. Strategic Collaborations and Ecosystem Expansion
- 8. Impact and Adoption of DeepHealth’s AI Solutions
- 9. Conclusion: The Future of Radiology with AI
- 10. References
In the modern digital healthcare environment, the role of FHIR data mapping, healthcare data interoperability, and FHIR integration is vital for improving healthcare outcomes and increasing operational efficiency [1]. However, healthcare data is often available in a disjointed format, stored across multiple systems, and is often a challenge for exchanging and standardizing this data.
Here, the role of FHIR (Fast Healthcare Interoperability Resources) is significant, and this is where healthcare interoperability and exchange standards, such as FHIR, become important. It is a modern healthcare data exchange standard that was developed by a health IT standards organization known as HL7 International.
What is FHIR?
FHIR stands for “Fast Healthcare Interoperability Resources” and is an interoperability standard that is widely used and accepted in the healthcare domain, allowing electronic data interchange using modern web technologies, especially RESTful APIs, JSON, and XML.
It is primarily intended to enable FHIR-based data integration, data exchange, and real-time data sharing in the healthcare domain.
At its core, FHIR is an interoperability standard that provides the following:
Resources are the core concept in FHIR, representing the data being exchanged, and are designed to support healthcare data mapping and transformation. The resources are as follows:
- Patient (data integration)
- Observation (data mapping)
- Medication (pharmacy data interoperability)
- Encounter (data exchange in the hospital domain) [2]
- Practitioner (data standardization)
Why FHIR Matters in the Realm of Healthcare Data
Healthcare systems are challenged by interoperability issues in health care data integration and standardization of clinical data. FHIR addresses these challenges in the following ways:
1. Standardization
FHIR offers a standard approach to the structure of health care data mapping and facilitates the proper understanding of the mapped health care data.
2. Interoperability
FHIR supports the integration of health care systems in a seamless manner and ensures the effective interoperability of electronic health records systems and health care applications like mobile health applications and health care analytics systems [3].
3. Flexibility
FHIR supports the implementation of simple and complex use cases of FHIR in a simple manner, including real-time use cases of FHIR.
4. Modern Integration
FHIR supports API-driven architecture and is therefore suitable for use in the development of cloud-based health care systems and AI-driven health care analytics
What is Data Mapping in Healthcare?
Data mapping in healthcare is the process through which data is mapped between two systems to ensure the accurate exchange of data.
Data mapping is an integral part of the following processes:
- Integration of EHR data
- Data transformation
- Healthcare data migration [4]
- Medical data standardization
Data mapping is vital in the following healthcare data exchanges:
- Electronic Health Records (EHRs) data mapping
- Laboratory Information Systems (LIS) data mapping
- Revenue cycle and billing data mapping
- Clinical trial data mapping
Without data mapping in healthcare, organizations are exposed to data inconsistencies and inaccuracies.
How FHIR is Used in Data Mapping
FHIR simplifies and improves healthcare data mapping applications through a structured and standardized approach.
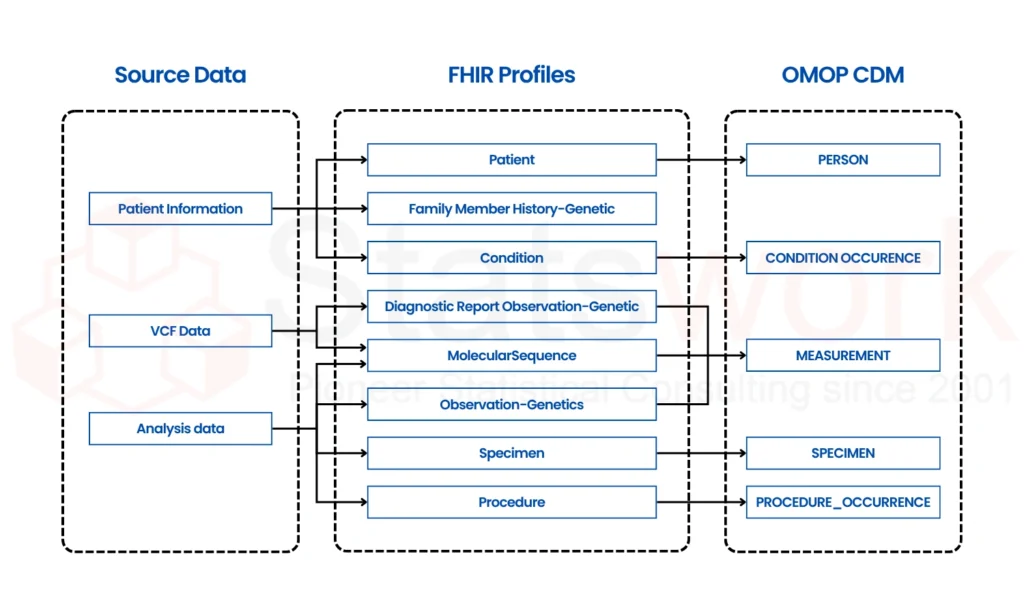
1. Mapping Legacy Data to FHIR Resources
Healthcare organizations require mapping legacy data to new and improved formats. FHIR helps healthcare organizations map legacy system data to new formats such as HL7 v2 and CDA.
Example:
HL7 v2 patient information → FHIR Patient
CDA documents → FHIR Observation
2. Semantic Interoperability
FHIR supports standardized medical terminologies such as SNOMED CT, LOINC, and ICD, thus facilitating semantic data mapping [3].
Benefit:
This ensures data accuracy.
3. API-Based Data Transformation
FHIR facilitates API-based data exchange in healthcare, thus making real-time data integration possible.
The mapping process involves:
- Extracting data
- Transforming data into FHIR data standards
- Delivering data through APIs
This facilitates real-time data integration, thus enabling timely decision-making.
4. Data Normalization
FHIR normalizes inconsistent data and standardizes it to a single data format, thus improving data quality and governance in healthcare [4].
Examples:
Date formats → ISO standards
Naming conventions → standard fields
This improves data normalization in healthcare systems.
5. Integration Across Multiple Systems
FHIR provides a single layer for integrating multiple healthcare systems, thus reducing multiple integrations.
Examples:
Health Information Exchange
Multi-hospital systems
AI and machine learning systems
This allows for an integration of architecture based on FHIR.
Benefits of Using FHIR Data Mapping
| Improved Accuracy | FHIR data mapping reduces errors in the transformation of healthcare data. |
| Faster Integration | FHIR data mapping enables the rapid integration of the FHIR API. |
| Scalability | FHIR data mapping allows the creation of reusable FHIR data models |
| Regulatory Compliance | FHIR data mapping enables the secure exchange of data, which follows HIPAA. |
Real-World Applications of FHIR Data Mapping
1. Electronic Health Record Integration
FHIR data mapping enables seamless EHR interoperability.
2. Clinical Research and Trials
FHIR data mapping enables the standardization of clinical data mapping.
3. AI & Machine Learning in Healthcare
FHIR data mapping enables the performance of machine learning models [2].
4. Mobile Health Applications
FHIR data mapping enables the secure access of patient data via the FHIR API.
Challenges in FHIR Data Mapping
Despite the benefits, there are challenges to be faced while implementing FHIR data mapping solutions:
- Complexity of Legacy Systems Legacy systems are complex and make healthcare data transformation a challenge.
- Terminology Alignment Requires knowledge of clinical coding standards [3].
- Data Quality Issues Data quality is a major issue, and poor quality may affect the correctness of FHIR mapping.
- Implementation Effort Requires highly skilled people to implement and integrate FHIR.
Best Practices for Effective FHIR Data Mapping
To ensure a successful healthcare data integration process through FHIR, the following best practices need to be followed:
- Data Profiling and Analysis
- Standardized Clinical Terminology
- Data Validation and Quality
- Automated FHIR Mapping
Conclusion
FHIR technology has significantly changed the face of data mapping and data interoperability in healthcare systems. It allows for a more standardized and API-based approach to data mapping and integration.
FHIR data mapping solutions have been beneficial for healthcare systems in terms of data integration, data interoperability, compliance, and scalability. With the changing face of digital healthcare, FHIR technology is here to stay for a long time.
Ready to streamline your healthcare data with FHIR?
Connect with us today and transform your data into seamless, interoperable insights.
Reference
- Brant, E. B., Kennedy, J. N., King, A. J., Gerstley, L. D., Mishra, P., Schlessinger, D., … & Liu, V. X. (2022). Developing a shared sepsis data infrastructure: a systematic review and concept map to FHIR. NPJ Digital Medicine, 5(1), 44. https://www.nature.com
- Baker, R. L., Hamidi, M., McKenzie, L., Denney, C. K., Edgar, T. D., Baker, R., & Edgar, T. (2023). The Story Behind the HL7 FHIR to CDISC Mapping Implementation Guide. Journal of the Society for Clinical Data Management, 4(1). https://www.jscdm.org
- Pfaff, E. R., Champion, J., Bradford, R. L., Clark, M., Xu, H., Fecho, K., … & Ahalt, S. (2019). Fast healthcare interoperability resources (FHIR) as a meta model to integrate common data models: development of a tool and quantitative validation study. JMIR medical informatics, 7(4), e15199. https://medinform.jmir.org
- Amar, F., April, A., & Abran, A. (2024). Electronic health record and semantic issues using fast healthcare interoperability resources: systematic mapping review. Journal of medical Internet research, 26, e45209. https://www.jmir.org/2024
- Andersen, B., Kasparick, M., Ulrich, H., Schlichting, S., Golatowski, F., Timmermann, D., & Ingenerf, J. (2016, October). Point-of-care medical devices and systems interoperability: A mapping of ICE and FHIR. In 2016 IEEE Conference on Standards for Communications and Networking (CSCN)(pp. 1-5). IEEE. https://ieeexplore.ieee.org